Business Name: BeeHive Homes of Grain Valley
Address: 101 SW Cross Creek Dr, Grain Valley, MO 64029
Phone: (816) 867-0515
BeeHive Homes of Grain Valley
At BeeHive Homes of Grain Valley, Missouri, we offer the finest memory care and assisted living experience available in a cozy, comfortable homelike setting. Each of our residents has their own spacious room with an ADA approved bathroom and shower. We prepare and serve delicious home-cooked meals every day. We maintain a small, friendly elderly care community. We provide regular activities that our residents find fun and contribute to their health and well-being. Our staff is attentive and caring and provides assistance with daily activities to our senior living residents in a loving and respectful manner. We invite you to tour and experience our assisted living home and feel the difference.
101 SW Cross Creek Dr, Grain Valley, MO 64029
Business Hours
Monday thru Saturday: Open 24 hours
Facebook: https://www.facebook.com/BeeHiveGV
Instagram: https://www.instagram.com/beehivegrainvalley/
The households I fulfill rarely get here with easy questions. They come with a patchwork of medical notes, a list of favorite foods, a child's contact number circled around twice, and a lifetime's worth of routines and hopes. Assisted living and the wider landscape of senior care work best when they respect that complexity. Individualized care plans are the framework that turns a structure with services into a place where someone can keep living their life, even as their requirements change.
Care plans can sound clinical. On paper they consist of medication schedules, mobility support, and keeping track of procedures. In practice they work like a living biography, upgraded in genuine time. They record stories, preferences, activates, and goals, then translate that into daily actions. When succeeded, the strategy secures health and wellness while protecting autonomy. When done improperly, it becomes a checklist that deals with symptoms and misses the person.
What "customized" really needs to mean
A great plan has a few apparent ingredients, like the best dosage of the right medication or an accurate fall risk evaluation. Those are non-negotiable. But customization shows up in the information that seldom make it into discharge papers. One resident's high blood pressure rises when the room is noisy at breakfast. Another eats much better when her tea arrives in her own flower mug. Somebody will shower quickly with the radio on low, yet declines without music. These appear little. They are not. In senior living, small options compound, day after day, into mood stability, nutrition, self-respect, and fewer crises.
The finest plans I have seen read like thoughtful contracts instead of orders. They state, for example, that Mr. Alvarez chooses to shave after lunch when his trembling is calmer, that he invests 20 minutes on the outdoor patio if the temperature level sits between 65 and 80 degrees, which he calls his daughter on Tuesdays. None of these notes decreases a lab outcome. Yet they reduce agitation, improve cravings, and lower the problem on staff who otherwise think and hope.
Personalization begins at admission and continues through the full stay. Families in some cases expect a repaired file. The much better mindset is to treat the plan as a hypothesis to test, fine-tune, and often replace. Needs in elderly care do not stall. Mobility can alter within weeks after a minor fall. A brand-new diuretic might alter toileting patterns and sleep. A modification in roommates can agitate somebody with mild cognitive disability. The strategy needs to anticipate this fluidity.
The building blocks of an efficient plan
Most assisted living communities collect comparable information, however the rigor and follow-through make the difference. I tend to try to find 6 core elements.
- Clear health profile and danger map: medical diagnoses, medication list, allergic reactions, hospitalizations, pressure injury threat, fall history, discomfort indications, and any sensory impairments. Functional evaluation with context: not only can this person shower and dress, but how do they prefer to do it, what devices or triggers aid, and at what time of day do they function best. Cognitive and emotional baseline: memory care needs, decision-making capability, triggers for stress and anxiety or sundowning, chosen de-escalation methods, and what success appears like on an excellent day. Nutrition, hydration, and routine: food preferences, swallowing threats, dental or denture notes, mealtime routines, caffeine intake, and any cultural or spiritual considerations. Social map and significance: who matters, what interests are real, past functions, spiritual practices, preferred ways of adding to the community, and topics to avoid. Safety and communication strategy: who to require what, when to escalate, how to document changes, and how resident and household feedback gets captured and acted upon.
That list gets you the skeleton. The muscle and connective tissue come from a couple of long conversations where staff put aside the form and just listen. Ask someone about their most difficult early mornings. Ask how they made big decisions when they were younger. That might appear unimportant to senior living, yet it can reveal whether an individual worths independence above comfort, or whether they lean toward regular over range. The care strategy need to show these worths; otherwise, it trades short-term compliance for long-lasting resentment.
Memory care is customization showed up to eleven
In memory care areas, customization is not a benefit. It is the intervention. 2 homeowners can share the exact same medical diagnosis and phase yet require significantly different techniques. One resident with early Alzheimer's may love a consistent, structured day anchored by an early morning walk and a picture board of family. Another may do much better with micro-choices and work-like tasks that harness procedural memory, such as folding towels or arranging hardware.
I remember a guy who ended up being combative throughout showers. We tried warmer water, various times, same gender caregivers. Minimal improvement. A daughter casually mentioned he had actually been a farmer who began his days before daybreak. We shifted the bath to 5:30 a.m., introduced the fragrance of fresh coffee, and used a warm washcloth first. Aggression dropped from near-daily to practically none across three months. There was no brand-new medication, just a plan that respected his internal clock.
In memory care, the care plan should forecast misunderstandings and build in de-escalation. If someone thinks they require to get a kid from school, arguing about time and date hardly ever helps. A much better strategy offers the ideal reaction phrases, a brief walk, a comforting call to a relative if needed, and a familiar task to land the person in today. This is not hoax. It is compassion calibrated to a brain under stress.
The finest memory care strategies also acknowledge the power of markets and smells: the bakery scent machine that wakes hunger at 3 p.m., the basket of locks and knobs for agitated hands, the old church hymns at low volume throughout sundowning hour. None of that appears on a generic care list. All of it belongs on a personalized one.
Respite care and the compressed timeline
Respite care compresses whatever. You have days, not weeks, to learn habits and produce stability. Households use respite for caretaker relief, healing after surgery, or to test whether assisted living might fit. The move-in typically occurs under stress. That magnifies the value of tailored care because the resident is handling modification, and the household brings concern and fatigue.
A strong respite care plan does not aim for perfection. It goes for 3 wins within the very first 48 hours. Maybe it is uninterrupted sleep the first night. Perhaps it is a complete breakfast eaten without coaxing. Perhaps it is a shower that did not feel like a battle. Set those early goals with the household and then record precisely what worked. If somebody eats better when toast shows up first and eggs later on, capture that. If a 10-minute video call with a grandson steadies the mood at dusk, put it in the routine. Excellent respite programs hand the family a short, practical after-action report when the stay ends. That report typically ends up being the backbone of a future long-lasting plan.
Dignity, autonomy, and the line between safety and restraint
Every care plan negotiates a limit. We want to avoid falls but not paralyze. We want to ensure medication adherence but avoid infantilizing suggestions. We want to keep an eye on for wandering without stripping personal privacy. These compromises are not hypothetical. They show up at breakfast, in the corridor, and throughout bathing.
A resident who demands utilizing a walking stick when a walker would be more secure is not being tough. They are attempting to hold onto something. The plan ought to name the danger and design a compromise. Maybe the walking stick remains for short strolls to the dining room while staff sign up with for longer walks outside. Perhaps physical therapy concentrates on balance work that makes the walking stick more secure, with a walker offered for bad days. A strategy that reveals "walker just" without context might decrease falls yet spike depression and resistance, which then increases fall danger anyhow. The goal is not no danger, it is long lasting security aligned with a person's values.
A comparable calculus applies to alarms and sensing units. Innovation can support safety, but a bed exit alarm that shrieks at 2 a.m. can disorient someone in memory care and wake half the hall. A much better fit may be a silent alert to staff combined with a motion-activated night light that cues orientation. Personalization turns the generic tool into a gentle solution.
Families as co-authors, not visitors
No one knows a resident's life story like their family. Yet households in some cases feel dealt with as informants at move-in and as visitors after. The greatest assisted living communities treat families as co-authors of the plan. That requires structure. Open-ended invites to "share anything valuable" tend to produce polite nods and little data. Assisted questions work better.
Ask for 3 examples of how the person dealt with stress at various life stages. Ask what taste of support they accept, pragmatic or nurturing. Inquire about the last time they shocked the family, for much better or worse. Those answers offer insight you can not get from vital indications. They assist staff anticipate whether a resident reacts to humor, to clear logic, to peaceful existence, or to gentle distraction.
Families also need transparent feedback. A quarterly care conference with templated talking points can feel perfunctory. I favor much shorter, more frequent touchpoints connected to moments that matter: after a medication change, after a fall, after a vacation visit that went off track. The strategy evolves across those discussions. Over time, families see that their input develops visible changes, not simply nods in a binder.
Staff training is the engine that makes plans real
A customized plan implies absolutely nothing if individuals providing care can not execute it under pressure. Assisted living groups handle lots of citizens. Staff change shifts. New hires show up. A strategy that depends on a single star caregiver will collapse the first time that individual hires sick.
Training has to do four things well. Initially, it must equate the strategy into basic actions, phrased the way people actually speak. "Offer cardigan before helping with shower" is better than "enhance thermal convenience." Second, it must utilize repetition and circumstance practice, not just a one-time orientation. Third, it should show the why behind each option so personnel can improvise when scenarios shift. Finally, it needs to empower aides to propose strategy updates. If night personnel consistently see a pattern that day personnel miss out on, a good culture invites them to record and recommend a change.
Time matters. The neighborhoods that stick to 10 or 12 residents per caretaker during peak times can in fact personalize. When ratios climb up far beyond that, personnel go back to task mode and even the very best plan becomes a memory. If a facility claims detailed personalization yet runs chronically thin staffing, think the staffing.
Measuring what matters
We tend to determine what is easy to count: falls, medication mistakes, weight modifications, health center transfers. Those indications matter. Customization ought to enhance them over time. However some of the very best metrics are qualitative and still trackable.
I try to find how often the resident starts an activity, not just participates in. I watch how many rejections occur in a week and whether they cluster around a time or job. I keep in mind whether the very same caregiver manages hard minutes or if the strategies generalize across staff. I listen for how typically a resident uses "I" statements versus being spoken for. If someone begins to welcome their next-door neighbor by name again after weeks of quiet, that belongs in the record as much as a blood pressure reading.
These appear subjective. Yet over a month, patterns emerge. A drop in sundowning events after including an afternoon walk and protein snack. Fewer nighttime restroom calls when caffeine switches to decaf after 2 p.m. The plan evolves, not as a guess, however as a series of little trials with outcomes.
The cash conversation many people avoid
Personalization has a cost. Longer consumption assessments, staff training, more generous ratios, and specialized programs in memory care all need financial senior care beehivehomes.com investment. Households sometimes come across tiered rates in assisted living, where higher levels of care bring higher fees. It helps to ask granular questions early.
How does the community adjust pricing when the care strategy adds services like regular toileting, transfer support, or extra cueing? What takes place economically if the resident moves from basic assisted living to memory care within the same campus? In respite care, are there add-on charges for night checks, medication management, or transport to appointments?
The objective is not to nickel-and-dime, it is to line up expectations. A clear monetary roadmap prevents bitterness from structure when the strategy modifications. I have actually seen trust erode not when prices rise, but when they rise without a conversation grounded in observable needs and documented benefits.
When the plan fails and what to do next
Even the best plan will hit stretches where it merely stops working. After a hospitalization, a resident returns deconditioned. A medication that when stabilized mood now blunts hunger. A cherished buddy on the hall vacates, and solitude rolls in like fog.
In those minutes, the worst response is to press more difficult on what worked previously. The better move is to reset. Assemble the little team that knows the resident best, including family, a lead aide, a nurse, and if possible, the resident. Name what altered. Strip the plan to core goals, 2 or three at most. Develop back intentionally. I have actually enjoyed strategies rebound within 2 weeks when we stopped attempting to repair everything and focused on sleep, hydration, and one cheerful activity that belonged to the person long before senior living.
If the plan repeatedly stops working in spite of client modifications, consider whether the care setting is mismatched. Some people who get in assisted living would do much better in a devoted memory care environment with different cues and staffing. Others may require a short-term knowledgeable nursing stay to recuperate strength, then a return. Customization consists of the humbleness to suggest a various level of care when the proof points there.


How to assess a neighborhood's approach before you sign
Families visiting neighborhoods can sniff out whether individualized care is a slogan or a practice. During a tour, ask to see a de-identified care strategy. Look for specifics, not generalities. "Motivate fluids" is generic. "Offer 4 oz water at 10 a.m., 2 p.m., and with meds, flavored with lemon per resident preference" reveals thought.
Pay attention to the dining-room. If you see an employee crouch to eye level and ask, "Would you like the soup first today or your sandwich?" that informs you the culture values choice. If you see trays dropped with little conversation, customization might be thin.
Ask how strategies are updated. A good answer references ongoing notes, weekly evaluations by shift leads, and family input channels. A weak answer leans on annual reassessments only. For memory care, ask what they do throughout sundowning hour. If they can describe a calm, sensory-aware regimen with specifics, the plan is most likely living on the flooring, not just the binder.
Finally, try to find respite care or trial stays. Neighborhoods that provide respite tend to have stronger intake and faster personalization since they practice it under tight timelines.
The quiet power of regular and ritual
If personalization had a texture, it would seem like familiar fabric. Rituals turn care tasks into human minutes. The headscarf that indicates it is time for a walk. The photo positioned by the dining chair to hint seating. The method a caregiver hums the first bars of a preferred tune when assisting a transfer. None of this expenses much. All of it needs understanding a person all right to choose the best ritual.
There is a resident I consider often, a retired librarian who safeguarded her independence like a valuable very first edition. She refused assist with showers, then fell two times. We developed a strategy that gave her control where we could. She picked the towel color each day. She marked off the steps on a laminated bookmark-sized card. We warmed the restroom with a little safe heating system for three minutes before starting. Resistance dropped, therefore did threat. More importantly, she felt seen, not managed.
What personalization gives back
Personalized care strategies make life simpler for staff, not harder. When regimens fit the individual, rejections drop, crises diminish, and the day streams. Families shift from hypervigilance to collaboration. Citizens spend less energy defending their autonomy and more energy living their day. The measurable results tend to follow: fewer falls, less unnecessary ER trips, better nutrition, steadier sleep, and a decrease in behaviors that lead to medication.
Assisted living is a guarantee to balance assistance and self-reliance. Memory care is a pledge to hang on to personhood when memory loosens up. Respite care is a promise to give both resident and family a safe harbor for a brief stretch. Personalized care plans keep those promises. They honor the particular and equate it into care you can feel at the breakfast table, in the quiet of the afternoon, and throughout the long, sometimes uncertain hours of evening.
The work is detailed, the gains incremental, and the effect cumulative. Over months, a stack of little, accurate choices ends up being a life that still looks and feels like the resident's own. That is the function of personalization in senior living, not as a luxury, but as the most useful path to dignity, security, and a day that makes sense.
BeeHive Homes of Grain Valley provides assisted living care
BeeHive Homes of Grain Valley provides memory care services
BeeHive Homes of Grain Valley provides respite care services
BeeHive Homes of Grain Valley offers 24-hour support from professional caregivers
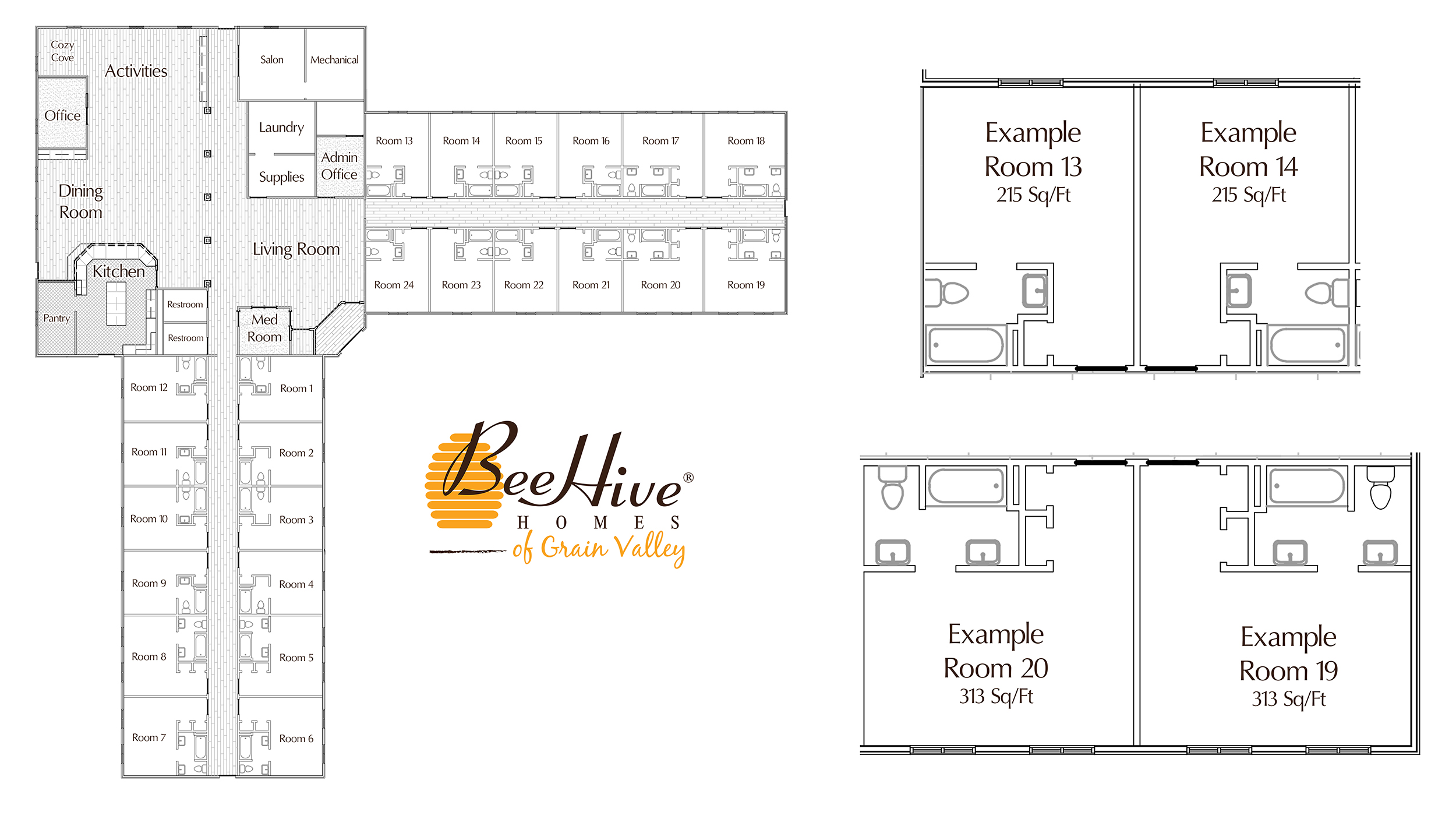
BeeHive Homes of Grain Valley offers private bedrooms with private bathrooms
BeeHive Homes of Grain Valley provides medication monitoring and documentation
BeeHive Homes of Grain Valley serves dietitian-approved meals
BeeHive Homes of Grain Valley provides housekeeping services
BeeHive Homes of Grain Valley provides laundry services
BeeHive Homes of Grain Valley offers community dining and social engagement activities
BeeHive Homes of Grain Valley features life enrichment activities
BeeHive Homes of Grain Valley supports personal care assistance during meals and daily routines
BeeHive Homes of Grain Valley promotes frequent physical and mental exercise opportunities
BeeHive Homes of Grain Valley provides a home-like residential environment
BeeHive Homes of Grain Valley creates customized care plans as residents’ needs change
BeeHive Homes of Grain Valley assesses individual resident care needs
BeeHive Homes of Grain Valley accepts private pay and long-term care insurance
BeeHive Homes of Grain Valley assists qualified veterans with Aid and Attendance benefits
BeeHive Homes of Grain Valley encourages meaningful resident-to-staff relationships
BeeHive Homes of Grain Valley delivers compassionate, attentive senior care focused on dignity and comfort
BeeHive Homes of Grain Valley has a phone number of (816) 867-0515
BeeHive Homes of Grain Valley has an address of 101 SW Cross Creek Dr, Grain Valley, MO 64029
BeeHive Homes of Grain Valley has a website https://beehivehomes.com/locations/grain-valley
BeeHive Homes of Grain Valley has Google Maps listing https://maps.app.goo.gl/TiYmMm7xbd1UsG8r6
BeeHive Homes of Grain Valley has Facebook page https://www.facebook.com/BeeHiveGV
BeeHive Homes of Grain Valley has an Instagram page https://www.instagram.com/beehivegrainvalley/
BeeHive Homes of Grain Valley won Top Assisted Living Homes 2025
BeeHive Homes of Grain Valley earned Best Customer Service Award 2024
BeeHive Homes of Grain Valley placed 1st for Senior Living Communities 2025
People Also Ask about BeeHive Homes of Grain Valley
What is BeeHive Homes of Grain Valley monthly room rate?
The rate depends on the level of care needed and the size of the room you select. We conduct an initial evaluation for each potential resident to determine the required level of care. The monthly rate ranges from $5,900 to $7,800, depending on the care required and the room size selected. All cares are included in this range. There are no hidden costs or fees
Can residents stay in BeeHive Homes of Grain Valley until the end of their life?
Usually yes. There are exceptions, such as when there are safety issues with the resident, or they need 24 hour skilled nursing services
Does BeeHive Homes of Grain Valley have a nurse on staff?
A consulting nurse practitioner visits once per week for rounds, and a registered nurse is onsite for a minimum of 8 hours per week. If further nursing services are needed, a doctor can order home health to come into the home
What are BeeHive Homes of Grain Valley's visiting hours?
The BeeHive in Grain Valley is our residents' home, and although we are here to ensure safety and assist with daily activities there are no restrictions on visiting hours. Please come and visit whenever it is convenient for you
Do we have couple’s rooms available?
Yes, each home has rooms designed to accommodate couples. Please ask about the availability of these rooms
Where is BeeHive Homes of Grain Valley located?
BeeHive Homes of Grain Valley is conveniently located at 101 SW Cross Creek Dr, Grain Valley, MO 64029. You can easily find directions on Google Maps or call at (816) 867-0515 Monday through Sunday Open 24 hours
How can I contact BeeHive Homes of Grain Valley?
You can contact BeeHive Homes of Grain Valley by phone at: (816) 867-0515, visit their website at https://beehivehomes.com/locations/grain-valley, or connect on social media via Facebook or Instagram
You might take a short drive to Sinclair's Restaurant. Sinclair’s Restaurant provides familiar comfort food that supports enjoyable assisted living or memory care dining experiences during respite care outings.